“If signs or symptoms consistent with DCS develop, initiate appropriate first aid and contact the nearest emergency medical services. For additional emergency assistance contact DAN +1-919-684-9111.”
There are several elements to the effective management of DCS, specifically on-the-scene evaluation and first aid, transport and definitive medical evaluation and treatment. Anyone who has suffered DCS should seek appropriate evaluation, and possibly ongoing care, from a physician well informed about diving-related medical issues.
In this chapter, you’ll learn about:
- On-the-Scene First Aid
- Subsequent Evaluation
- Hyperbaric Oxygen Therapy
- In-Water Recompression
- Emergency Resources
On-the-Scene First Aid
The foundation of first aid is basic life support. The primary first aid measure for DCS is delivery of supplemental oxygen in the highest concentration, or fraction, that is practical (Longphre et al. 2007). High oxygen fractions, if provided rapidly and over a sustained period, can reduce or even eliminate symptoms of DCS, albeit often only temporarily if definitive treatment is not secured. Continuous-flow oxygen systems, using non-rebreather or pocket masks, are frequently available in diving environs; however, such equipment delivers modest oxygen fractions. Much higher fractions can be achieved with demand masks, though they are appropriate only for conscious individuals able to breathe on their own.
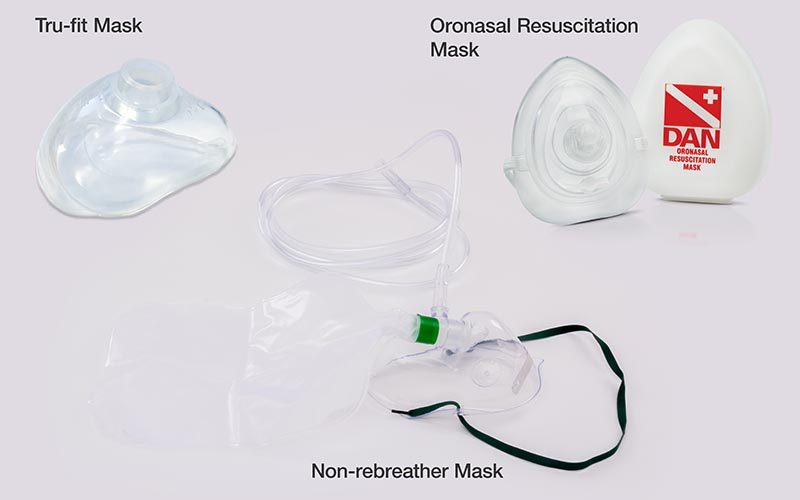
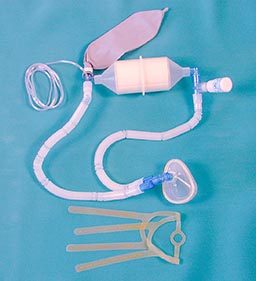
Rebreather systems are another on-the-scene option; such systems permit the unused oxygen in the diver’s exhalations to be recycled, or rebreathed. A rebreather apparatus can thus provide high fractions with minimal gas use and may prove especially helpful in settings where the supply of oxygen is limited (Pollock 2004; Pollock and Natoli 2007).
Chemical oxygen generating systems — devices with a long shelf life that deliver oxygen via a chemical reaction — may in some situations be the only option available. However, if emergency medical services are not readily accessible, such devices are unlikely to provide a sufficient oxygen supply (Pollock and Natoli 2010).
Subsequent Evaluation
First aid is just the first step in treating an affected diver. Anyone who has experienced symptoms associated with DCS is advised to seek subsequent medical evaluation. This should occur even if the diver’s symptoms improved or disappeared upon the administration of oxygen, since subtle issues can be missed or symptoms can return once oxygen delivery is stopped. For the same reason, it is advisable to seek input from an experienced dive-medicine specialist — someone aware of all the nuances in the presentation, course and treatment of DCS.
Hyperbaric Oxygen Therapy
The definitive treatment for DCS is hyperbaric oxygen (HBO) therapy, or the delivery of pure oxygen at a pressure substantially higher than that of atmospheric pressure. HBO therapy reduces the size of any bubbles and improves gradients which promote oxygen delivery and inert gas elimination. HBO therapy is typically delivered in recompression chambers.

A common HBO regimen is the U.S. Navy Treatment Table 6 (USN 2008). According to this regimen, the hyperbaric chamber is initially pressurized to 2.8 atmospheres absolute (ATA), equivalent to the pressure found at 60 feet (18 meters) of seawater. The patient breathes pure oxygen, interspersed with scheduled periods of breathing regular air to reduce the risk of oxygen toxicity. The usual duration of the USN TT6 treatment is just under five hours, but extensions can be added as required, based on the patient’s response.

HBO treatment can be conducted in a monoplace chamber, often an acrylic tube sized to hold just one patient, or in a multiplace chamber, sized to accommodate one or more patients plus one or more “tenders” — that is, technicians or other medical personnel. Multilock chambers are designed to allow patients, tenders or equipment to be transferred into and out of the chamber while treatment is ongoing.
The course of HBO therapy will vary according to the particulars of each case; both the presentation of DCS and its response to treatment can be idiosyncratic. A full resolution of DCS symptoms can often be achieved with one or sometimes multiple HBO treatments. In some cases, however, resolution will be incomplete, even after many treatments. The normal clinical approach is to continue the treatments until no further improvement is seen in the patient’s symptoms. Modest residual symptoms will then often resolve slowly, after the treatment series is ended. Full resolution of symptoms can sometimes take months to achieve and in some instances may never be realized.

In-Water Recompression

In-water recompression may be an alternative to chamber recompression in remote locations, if there is neither a nearby chamber nor the means to quickly transport the patient to a chamber elsewhere. The technique involves bringing the diver underwater again, to drive gas bubbles back into solution to reduce symptoms and then slowly decompress in a way that maintains an orderly elimination of the excess gas.
While in-water recompression is simple in concept, it is practical only with a substantial amount of planning, support, equipment and personnel; appropriate water conditions; and suitable patient status. Critical challenges can arise due to changes in the patient’s consciousness, oxygen toxicity, gas supply, and even thermal stress. An unsuccessful in-water recompression may leave the patient in worse shape than had the attempt not been made. The medical and research communities are divided on the utility of in-water recompression. It is beyond the scope of this publication to consider all of the relevant factors, but it is fair to say that there are probably more situations when in-water recompression should not be undertaken than situations when it would be a reasonable choice.
As a general rule, a diver who develops symptoms consistent with DCS should be removed from the water, and first aid should be delivered on the surface, even if there is likely to be a delay before definitive medical care can be sought.
Emergency Resources
The best course of action, if signs or symptoms consistent with DCS (or any other serious injury) develop, is to initiate appropriate first aid and then immediately contact the nearest emergency medical services (EMS). The next step should be to contact DAN to seek advice regarding the proper progression of care. The organization’s emergency hotline number is +1-919-684-9111.
It is generally not appropriate to show up unannounced at the nearest hyperbaric chamber. This could mean bypassing a facility where the victim might be able to receive a more thorough and appropriate evaluation. Remember that not all injuries associated with diving are DCS, even if it seems so in the heat of the moment. In addition, the chambers at some facilities are not available to treat divers at all times or ever. One of the challenges within North America is the shrinking number of hyperbaric chambers that accept diving casualties, particularly outside normal business hours.
The key point to remember is that establishing contact with emergency medical services and DAN can ensure timely and appropriate case management. When in doubt, call.
WHEN YOU CALL THE
DAN EMERGENCY HOTLINE
- Tell the operator you have a dive emergency. The operator will confirm your name, location and phone number, and ether connect you directly with DAN medical staff or have someone call you back at the earliest possible moment.
- The medical staff member may make an immediate recommendation or call you back after making arrangements with a local physician
- The medical staff member may ask you to wait by the phone while arrangements are being made. These plans may take 30 minutes or longer, as complex coordination is often required. If the situation is life-threatening, arrange safe transport for the diver to the nearest medical facility for immediate stabilization and assessment first. Then call the DAN Emergency Hotline for consultation with the local medical provider.
Even if symptoms were not severe and they resolved completely, a diver who has had multiple bouts of DCS must take special considerations. Especially if DCS is recurring following otherwise safe dive profiles, a dive medical specialist must be consulted to determine if diving can be resumed safely.
DAN EMERGENCY HOTLINE +1 919-684-9111
Next: Chapter 5 – Factors Contributing to Decompression Stress >
