Immersion, cold water, hyperoxia, exercise or the work of breathing on a Closed-Circuit Rebreather could challenge the cardiopulmonary system. The purpose of this study was to examine the impact of CCR diving on lung function and autonomous cardiac activity after a series of CCR dives in cold water.
If we focus on the lung function, previous studies have shown that an increase in the work of breathing (WOB), especially with a negative pressure, can increase extravascular lung water (Castagna et al, 2018), which is reflected by the appearance of B lines (figure 1) on the echography, which testify to a loss of pulmonary aeration… That lung function could also be transitorily altered after deep CCR dives with a loss of Forced Vital Capacity (FVC) about 30% (Dugrenot et al, 2021), but the link between the 2 has not yet been shown.
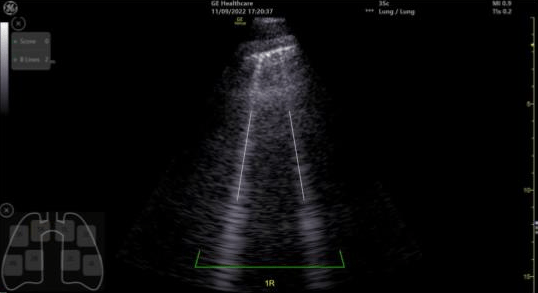
Figure1: example of B lines on a pulmonary echography
Regarding to the cardiac function, global Heart Rate Variability (HRV) modifications during diving may highlight physiological constraints as well as environmental-stress-related stimulation that may influence pulmonary changes.
This experimental study was completed in 2022.
The use of closed-circuit rebreathers (CCR) has become increasingly common in the recreational scuba diving community over the past two decades. Their use allows longer and deeper dives than classical open-circuit (OC) scuba equipment. If CCRs bring major advantages in terms of autonomy and range of action, they also bring new technical challenges and constraints to the cardio-pulmonary system.
Among the different CCR configurations, the back mounted counter lungs CCR seem to be at greater risk factor to develop interstitial pulmonary oedema (while they are the most common on the market), as a study from Castagna et al, (2018) have shown increased B lines in both chest and back mounted CCR, with a higher score on back mounted CCR. Nevertheless, they were comparing divers in a horizontal position,
which does not really correspond to a CCR diver position, with a slightly modified trim (maximum 30-degree angle from horizontal trim), to limit a possible impact of a pressure delta on the work of breathing (WOB).

Before drawing any conclusions, it is also important to remember that even exercise itself can cause the appearance of B lines, even on healthy subjects (Simonovic et al, 2018) and that pressure variations could also impact B lines formation (Debevec et al, 2022).
Our goal in this study was then to evaluate the cardiopulmonary impact of repeated back mounted CCR dives in cold water: so, we have followed 8 CCR divers on a one-week diving trip in the Baltic Sea, and we
measured, among other things, spirometry parameters, oxygen saturation (SpO2), HRV, and the lung ultrasonography score (LUS), which reflects possible extravascular lung water.
Interestingly, if we did observe transient increased LUS after diving combined with a slight non-pathological decrease in oxygen saturation (SpO2), it doesn’t seem correlated with the depth, and it was not linked with any loss of FVC while the dives were held up to 230 feet of salt water (fsw) or 70 meters of salt water (msw).
To conclude, the lung aeration disorders observed seem to be transient and not associated with functional alteration which implies the impact of these impairments is unknown and should not be neglected until we better understand these IPE and the decreases in FVC observed during deep CCR dives.
Besides these cardiopulmonary parameters, the team also collaborated in another study focused on the inflammatory pathway related to decompression sickness (DCS), and more precisely on circulating microparticles, which are known to initiate a systemic inflammatory response. These microparticles were indeed increased after a deep CCR dive or after shallow repetitive CCR dives, highlighting inflammatory events decorrelated from the depth of diving.
Additional Reading References
Scientific articles
Gouin, Emmanuel, Costantino Balestra, Jeremy Orsat, Emmanuel Dugrenot, and Erwan L’Her. “Pulmonary Effects of One Week of Repeated Recreational Closed-Circuit Rebreather Dives in Cold Water.” Medicina 59, no. 1 (December 30, 2022): 81. https://doi.org/10.3390/medicina59010081.
·Arya, Awadhesh K., Costantino Balestra, Veena M. Bhopale, Laura J. Tuominen, Anne Räisänen-Sokolowski, Emmanuel Dugrenot, Erwan L’Her, Abid R. Bhat, and Stephen R. Thom. “Elevations of Extracellular Vesicles and Inflammatory Biomarkers in Closed Circuit SCUBA Divers.” International Journal of Molecular Sciences 24, no. 6 (March 22, 2023): 5969. https://doi.org/10.3390/ijms24065969.
Related publications
Castagna, Olivier, Jacques Regnard, Emmanuel Gempp, Pierre Louge, François Xavier Brocq, Bruno Schmid, Anne-Virginie Desruelle, et al. “The Key Roles of Negative Pressure Breathing and Exercise in the Development of Interstitial Pulmonary Edema in Professional Male SCUBA Divers.” Sports Medicine – Open 4, no. 1 (December 2018): 1. https://doi.org/10.1186/s40798-017-0116-x.
Debevec, Tadej, Mathias Poussel, Damjan Osredkar, Sarah J. Willis, Claudio Sartori, and Grégoire P. Millet. “Post-Exercise Accumulation of Interstitial Lung Water Is Greater in Hypobaric than Normobaric Hypoxia in Adults Born Prematurely.” Respiratory Physiology & Neurobiology 297 (March 2022): 103828. https://doi.org/10.1016/j.resp.2021.103828.
Dugrenot, Emmanuel, Costantino Balestra, Emmanuel Gouin, Erwan L’Her, and François Guerrero. “Physiological Effects of Mixed-Gas Deep Sea Dives Using a Closed-Circuit Rebreather:
A Field Pilot Study.” European Journal of Applied Physiology 121, no. 12 (December 2021): 3323–31. https://doi.org/10.1007/s00421-021-04798-y.
Simonovic, Dejan, Stefano Coiro, Erberto Carluccio, Nicolas Girerd, Marina Deljanin-Ilic, Gaia Cattadori, and Giuseppe Ambrosio. “Exercise Elicits Dynamic Changes in Extravascular Lung Water and Haemodynamic Congestion in Heart Failure Patients with Preserved Ejection Fraction: Exercise Elicits Dynamic Changes in Extravascular Lung Water and Haemodynamic Congestion in Heart Failure Patients with Preserved Ejection Fraction.” European Journal of Heart Failure 20, no. 9 (September 2018): 1366–69. https://doi.org/10.1002/ejhf.1228.