I had just turned 61 a few days earlier and was in great shape. Since I began diving in graduate school in the early 1990s, I had logged more than 1,000 dives, including my first tech dives. Back when I started tech diving we were still experimenting with gas mixes and protocols, but I had never been bent — not even a niggle — so I sure wasn’t expecting it that day.
The incident occurred when two friends and I were diving rebreathers on a subsea pinnacle off Point Lobos in Northern California. Conditions were pristine: The ocean was as still as a lake, there was no current, and visibility was in excess of 40-50 feet. My buddy and I hit a max depth of 101 feet and began slowly working our way back up the rocky pinnacle toward the surface.
The oxygen level on my rebreather was set at PO2=1.3 atm with air diluent, and we were well within our no-stop limits for the entire dive. At about 45 feet I experienced what felt like a sinus squeeze. I stopped, swallowed and wiggled my nose, and the feeling went away. I continued my ascent, made a 20-foot safety stop, surfaced after 57 minutes and climbed into the inflatable boat without incident. Everything was sublime.
Forty minutes later as I was driving home, I noticed the hearing in my left ear was distorted. Because I felt fine otherwise, I figured my ear was simply a little bit plugged up, but the distortion continued into the evening. When I awoke the next morning it was as if someone had placed a bowl over the left side of my head. I couldn’t hear anything in my left ear — nothing! I thought about calling DAN®, but given the innocuous dive profile and absence of other symptoms such dizziness or vertigo it seemed unlikely to me that my symptoms were dive related. In fact, what I was experiencing felt exactly like an impacted earwax blockage, which I’ve had before, so I went out and purchased an earwax removal kit and began treating myself.
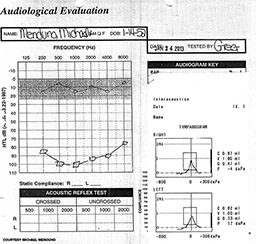
Five days later with no improvement in hearing, I saw Dr. Adam Marvin, an ear, nose and throat specialist who was also a diver. He examined my ear. There was no blockage, and no indications of barotrauma. Gulp. He gave me a hearing test. My left ear was nonfunctional across all frequencies. His diagnosis: profound sudden sensorineural hearing loss (SSHL), a spontaneous neurological condition that typically affects a single ear. There are about 4,000 cases a year in the U.S. and 150,000 worldwide. Most have no explainable cause.
Dr. Marvin told me there was no proven treatment for SSHL. As many as 50-65 percent of patients experience a spontaneous remission in two weeks, but in others there is no improvement — although some patients respond to oral corticosteroid therapy. He said there was no way of knowing whether my condition was dive related or not or whether my ear would improve. He suggested I consult a hyperbaric specialist, told me not to eat salt and prescribed a two-week regimen of very high doses of prednisone and Vitamin B.
Fearing permanent hearing loss, I immediately emailed my friend, hyperbaric physician Dr. Simon Mitchell, who chairs the anaesthesiology department at the University of Auckland in New Zealand. Dr. Mitchell wrote back and said that while idiopathic sudden sensorineural hearing loss was a possible explanation, it was highly likely that I was experiencing inner-ear decompression sickness (DCS), given the proximity of the occurrence to diving and the lack of signs of inner-ear barotrauma.
Though inner-ear DCS is typically associated with deep helium diving, it can also happen in shallow water. Dr. Mitchell, who had published on the subject, sent me a paper that concluded that not only can inner-ear DCS occur even in the absence of a decompression schedule violation, but it is also more common in recreational air diving than previously thought.1 In fact, 21 percent of the inner-ear DCS incidents reported occurred within the no-stop limits. And, although 86 percent of the cases involved vestibular symptoms such as vertigo, only 14 percent of the cases involved pure hearing loss only, and 97 percent occurred within two hours of the dive. The bad news? Most cases did not make a full recovery even with hyperbaric treatment. Dr. Mitchell recommended that I call DAN despite the fact it was now eight days after the injury.
The next day I spoke with a DAN medical information specialist who referred me to Dr. Paul Cianci, a former U.S. Navy diving medical officer who had helped to establish three hyperbaric centers in the San Francisco Bay area. He examined me 11 days post incident. The prednisone appeared to be having some effect; I was beginning to hear sound in my left ear, but I still could not recognize words.
Dr. Cianci explained that my condition could be SSHL or inner-ear DCS, adding that we still know very little about the workings of either condition. Fortunately, hyperbaric oxygen therapy was now a recommended protocol for SSHL, so either way my best option was chamber treatment.
Dr. Cianci prescribed an initial series of 10 treatments of 2 ATA of oxygen for 90 minutes daily (I breathed pure oxygen in a monoplace chamber pressurized to 2 ATA) in conjunction with continued hearing tests to determine the treatments’ effectiveness. Fortunately my hearing continued to improve both in terms of decibel sensitivity and word recognition. Despite some pushback from the insurance company Dr. Cianci added a second series of 10 treatments.
I was lucky. Though my left ear now has mild-to- moderate sensorineural loss in the low frequencies — things sound a bit tinny — my hearing is on the low end of “normal” in the mid- to high-frequency range.
The takeaway? Listen up. If you experience any abnormal symptoms following a dive, call DAN immediately. It can only improve your odds.
Reference
1. Nachum Z, et al. Inner Ear Decompression Sickness in Sport Compressed-Air Diving. Laryngoscope 2001; 111: 851-856.
© Alert Diver — Q1 Winter 2015