Many divers are unaware they have heart disease until they experience a medical incident. Divers Alert Network® (DAN®) recommends regular evaluations to detect hypertension and high cholesterol before they lead to a problem — in the water or out.
According to the American Heart Association (AHA), cardiovascular disease, including heart disease and stroke, is the leading cause of death globally with more than 17.3 million deaths each year. The three major risk factors are hypertension, high cholesterol and smoking.
Hypertension
Hypertension, also known as high blood pressure, is a common medical condition in the general population, and divers are not exempt. According to the U.S. Centers for Disease Control and Prevention (CDC) and the AHA:
- 78 million American adults (or 31 percent — almost 1 in 3) have hypertension.
- In only 47 percent (less than half) of those cases is the hypertension condition under control.
- 30 percent of American adults have prehypertension.
Blood pressure is a measure of the force with which blood pushes outward on the arterial walls. A blood-pressure reading is a ratio of two numbers:
- Systolic pressure (the top number): when your heart is beating and
- Diastolic pressure (the bottom number): when your heart is resting between beats.
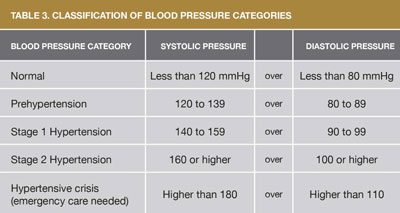
A normal blood pressure is 120/80 (stated as “120 over 80”). Hypertension is often diagnosed at 140/90 or above, but the criteria vary slightly from country to country. The table below shows the most common criteria used in the United States.
Hypertension comes with short-term and long-term complications. The most serious short-term complication is a “cerebrovascular accident,” a ruptured blood vessel in the brain, commonly known as a stroke. Long-term detrimental effects are more common and include coronary artery disease, kidney disease, congestive heart failure, eye problems and cerebrovascular disease.
Mild hypertension can often be controlled with diet and exercise; however, medication may be necessary to keep blood pressure within acceptable limits. Most antihypertensive drugs are compatible with diving, provided side effects are minimal; always seek the advice of a physician before engaging in physical activity.
- Antihypertensive drugs known as beta blockers may cause a decrease in maximum exercise capacity and may also affect the airways. These side effects typically do not cause problems for the average diver.
- Another class of antihypertensives, known as angiotensin-converting enzyme (ACE) inhibitors, may be preferred for divers, though a persistent cough is a possible side effect. As with any new medication, be sure you take it for at least a month before you dive with it.
- Calcium channel blockers are a third option. Side effects may include lightheadedness when standing up after sitting or lying down.
- Diuretics, drugs that promote urination, are also frequently used to treat hypertension. Their use requires ensuring adequate hydration and monitoring electrolyte levels in the blood.
Divers who can demonstrate adequate control of their blood pressure with no significant decrease in their in-water performance due to drug side effects should be able to dive safely. However, regular physical examinations are key and should include screening for long-term consequences of hypertension such as coronary artery disease.
High Cholesterol

Cholesterol is a soft, waxy substance found in blood that isn’t inherently bad. Hyperlipidemia, commonly known as high cholesterol, describes a condition in which the blood has excessive levels of lipids (fats) such as cholesterol and triglycerides.
Cholesterol is produced naturally by the liver and is used in the production of hormones. Consuming foods high in saturated fat and trans fat causes the liver to produce more cholesterol than it normally would. Cholesterol combines with proteins to form soluble lipoprotein particles. Lipoproteins come in two forms: low-density lipoprotein (LDL) and high-density lipoprotein (HDL).
LDL is considered “bad cholesterol” because when too much LDL builds up in the arteries’ inner walls it creates deposits, known as plaque, that can lead to narrowing and stiffening of the arteries. This condition is called atherosclerosis. It contributes to hypertension and can lead to peripheral artery disease, coronary artery disease, heart attack and stroke — as well as erectile dysfunction in men.
HDL cholesterol is considered “good cholesterol” because it transports cholesterol away from the bloodstream and back to the liver, which facilitates its removal from the body. HDL helps prevent the buildup of plaque in the arteries and reduces the risk of cardiovascular disease.
Triglycerides, a common type of fat, are another factor in hyperlipidemia. High triglyceride levels, combined with high levels of LDL cholesterol, increase one’s risk of cardiovascular disease.
An individual’s cholesterol level is a composite measure of LDL, HDL and triglycerides, in either milligrams per deciliter of blood (mg/dL) or millimoles per liter of blood (mmol/L). Many experts, including the National Institutes of Health and Mayo Clinic, recommend the following cholesterol levels:
- Total cholesterol: below 200 mg/dL (5.2 mmol/L)
- LDL cholesterol: below 130 mg/dL (3.4 mmol/L)
- HDL cholesterol: above 40 mg/dL (1 mmol/L) in men and above 50 mg/dL (1.3 mmol/L) in women
- Triglycerides: below 150 mg/dL (3.9 mmol/L)
Divers taking cholesterol-lowering (hypolipidemic) medications, such as Lipitor, Crestor or Zocor, should be aware of their side effects. Mu0scle pain is the most common side effect and may feel like aching, tiredness or weakness in the muscles. It’s important to note such symptoms before diving so they won’t be confused with symptoms of decompression sickness (DCS). If a diver develops new symptoms after a dive, assume a diving-related injury until a physician confirms otherwise.
Additional side effects that may interfere with diving include fatigue, difficulty or discomfort with breathing, digestive problems, cognitive dysfunction and/or increased blood sugar or type 2 diabetes. Also, certain conditions can intensify the side effects of statins. If you are over 65, take multiple medications, consume alcohol or have kidney or liver disease, you may be in a higher-risk group for side effects.
Regular exercise and a diet high in fiber and low in unhealthy fats are natural ways to combat high cholesterol.
Smoking
The World Health Organization (WHO) has called tobacco use “the single most preventable cause of death in the world today.” Smokers have a higher risk of coronary heart disease, stroke, peripheral artery disease and aortic aneurysm, and these risks greatly increase if the smoker has a family history of heart disease.
There are many benefits to quitting smoking. According to the National Health Service, just 72 hours after a smoker’s last cigarette:

- Carbon monoxide will be eliminated from the body.
- The lungs start to clear out mucus and other smoking debris.
- There is no nicotine in the body.
- The ability to taste and smell are improved.
- Breathing becomes easier.
- Bronchial tubes begin to relax, and energy levels increase.
Divers who don’t smoke should avoid inhaling smoke from those who do. According to the American Heart Association about 34,000 adults die each year from heart and blood-vessel disease caused by secondhand smoke. Nonsmokers exposed to secondhand smoke also have a 20-30 percent higher risk of stroke.
Take Care and Keep Diving
Heart disease is a common factor in diving fatalities. Although the overall fatality rate in scuba diving is relatively low, DAN researchers have found the risk of death while diving increases with age, mostly because of cardiac-health-related issues.
It’s never too early (or too late) to start taking care of your heart. By reducing lifestyle-related risk factors such as tobacco use, an unhealthy diet, physical inactivity and excessive alcohol consumption, you can enjoy the sport you love for decades to come.