The diver was a 54-year-old female. She was experienced (approximately 400 lifetime dives) and physically fit with no relevant medical history.
The Dives
She was on a weeklong dive vacation in the Caribbean and had been diving for two days with four dives each day. Her maximum depth was 90 feet. All dives were on air, and her bottom times were within her computer’s no-decompression limits. She spent at least one hour on the surface between dives and at least two hours between the morning and afternoon dives. After the last dive on the second day she began to feel soreness in her abdomen. She noticed areas of blotchiness that looked like bruising. The affected areas were tender, but in the deeper tissue rather than on the surface of her skin. She reported feeling as though she had done “too many sit-ups.” Some slight itching was present, but the soreness and discoloration were most prominent. Based on their previous experience, the dive staff believed this was the result of a sting by a marine animal.
The blotchiness resolved within two hours, but the soreness remained. It was mild enough, though, that she could enjoy dinner and a casual evening walk with her traveling companions. By the next morning the soreness was almost completely resolved, and she decided to participate in the morning dives.
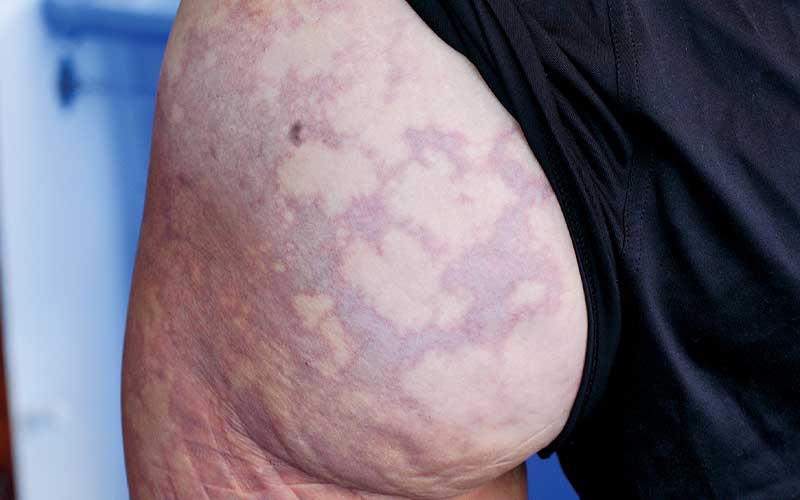
The first dive was an uneventful drift dive to 64 feet for 55 minutes. The abdominal pain increased following that dive. She attributed this increase to the physical activity of the dive. The next dive was to 58 feet for 50 minutes. Upon surfacing she experienced even more abdominal discomfort and soreness of both breasts. Upon removing her wetsuit she noticed the areas of blotching had returned, but they were darker and larger than those of the previous day. There were no blotches on her breasts, but they were very tender. The symptoms were again attributed to a sting or an allergic reaction to an unknown irritant. She had never experienced any symptoms like this on previous dives.
The dive boat returned to shore for lunch before the afternoon dives. Forty-five minutes after her last dive the blotchy areas seemed to be diminishing, but the diver began to complain of blurred vision, dizziness and general discomfort and malaise. Her companions realized she was confused regarding their location, and she had no memory of the morning’s dives. Her companions were alarmed and summoned the dive staff, who placed the diver on high-flow oxygen and arranged transport to the local hyperbaric clinic.
The Evaluation
Upon her arrival at the clinic, the hyperbaric physician examined her. After 20 minutes of breathing oxygen her memory was no longer impaired, and the dizziness and blurred vision had completely resolved. The blotchy areas had faded, but the abdominal and breast soreness was unchanged. The physician diagnosed her with Type II decompression sickness (DCS) and immediately initiated treatment in the chamber. She was treated with a U.S. Navy Treatment Table 6 (TT6). During the treatment all the blotchiness resolved, and the soreness in her abdomen and breasts was greatly reduced. Besides the residual soreness, her examination after the treatment was normal. The physician instructed her to return to the clinic the following morning for a follow-up exam.
The next morning her soreness was the same as it had been after the TT6. The physician treated her again — this time with a U.S. Navy Treatment Table 5, a shorter chamber treatment. The soreness was further reduced, and the physician recommended managing the residual soreness with ibuprofen. He also strongly advised against further diving. The soreness completely resolved over the next two days, and the diver flew home without any return of symptoms or other problems.
Discussion
When confronted with unfamiliar symptoms, many of us will try to relate the complaints to something familiar — even when the conclusion is unlikely. In this case, the dive staff assumed the diver’s symptoms resulted from a marine animal sting and didn’t consider or know of other possible explanations. Skin symptoms of DCS can mimic other conditions, but there are important aspects of “skin bends” that help distinguish it from other dermatological conditions. Divers may have heard skin bends described as similar to a rash or hives, but those with the condition tend to report dark, mottled areas that are not typically raised. A careful evaluation including review of medical history and dive profiles can provide further clarification. Itching, burning or other unusual sensations may be present but seem to occur less frequently. Deep-tissue soreness and tenderness are the most frequently reported symptoms along with areas that are bruised or blotchy. The surface of the skin may or may not be tender.
The exact cause and mechanism of skin bends is not clearly understood, and accurate predictors of individuals’ susceptibility do not yet exist. Based on the reports DAN® receives, the symptoms most commonly occur in areas of the body with the most fatty (adipose) tissue. This includes the abdomen, thighs, triceps area, buttocks and, in women, the breasts.
According to DAN Research, approximately 20 percent of divers who experience skin bends have accompanying neurological symptoms. This case illustrates the occurrence of such symptoms (confusion, visual blurring and memory loss). The diver’s presentation was alarming, and her companions recognized the seriousness. Any diver who presents with potential skin bends should be placed on oxygen and seek medical evaluation; neurological symptoms may be subtle.
While most cases of skin bends are relatively mild, decompression sickness is worth avoiding, and there are some basic strategies that may help reduce the likelihood of symptom occurrence. Using nitrox while diving air tables (or setting your computer to “air”) will reduce the nitrogen load (depth limits must always be observed when using nitrox). If you’re breathing air, shorten bottom times by five to 10 minutes and consider prolonging safety stops beyond three minutes. Divers who experience repeated episodes of DCS should seek a thorough evaluation by a physician trained in dive medicine.
Early recognition of symptoms is very important. If signs or symptoms of DCS occur, suspend all diving, initiate oxygen therapy, and seek medical attention. Breathing oxygen on the surface can provide remarkable improvement, but a physician must determine whether further treatment is necessary. Even if mild soreness is the only symptom, further diving is extremely likely to cause symptoms to recur or worsen. If you have any unusual symptoms after diving, do not hesitate to call the DAN Emergency Hotline (+1-919-684-9111) to discuss the situation.
© Alert Diver — Q2 Spring 2012