David Fothergill’s research helps divers and submariners.
A research physiologist with an impressive publication record covering mostly diving and naval medicine, David M. Fothergill, Ph.D., is the scientific director for the Naval Submarine Medical Research Laboratory (NSMRL) based at Naval Submarine Base New London in Groton, Connecticut. After he earned a degree in sports science at Liverpool John Moores University in England, his interest in diving physiology sparked during his kinesiology master’s thesis work in hyperbaric physiology at Simon Fraser University in British Columbia, Canada. While there, he discovered his passion for diving and got his first certification diving off the eastern shore of Vancouver Island. Following completion of his doctorate in occupational biomechanics at the Royal Free Hospital School of Medicine in London, England, he worked for the Naval Medical Research Institute in Maryland, specializing in diving physiology before his focus broadened to include submariners and submarine medicine at NSMRL.

Tell us about where you work at the Naval Submarine Base New London.
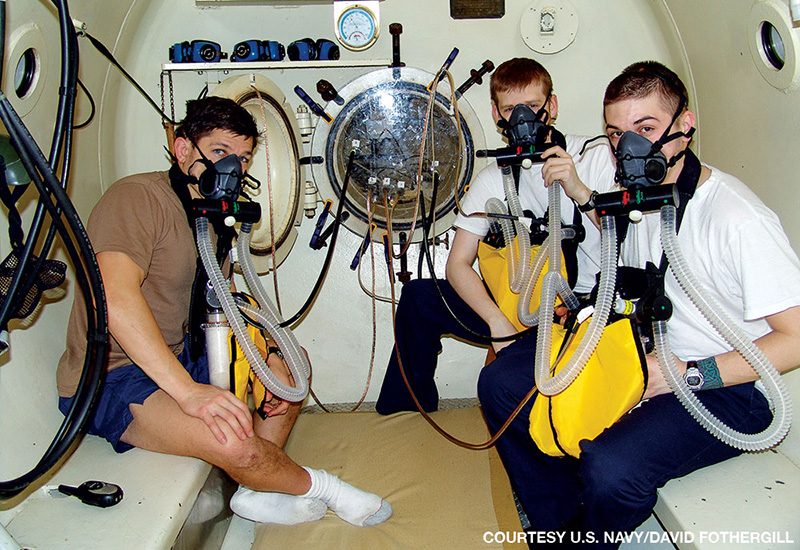
The NSMRL is a military command under the Bureau of Medicine and Surgery. Its mission is the welfare, health and performance of the undersea warfighter, which includes both submariners and divers. Around 70 people with varying backgrounds work here, including military, civil servants and contractors. There are physiologists, physicians, psychologists, engineers and support staff as well as a full dive locker and the historic Genesis hyperbaric chamber, which researchers have used for numerous studies over the past 50 years, including saturation diving experiments in the 1960s.
Besides being one of the U.S. Navy’s home bases for fast-attack submarines, New London houses training commands that prepare new submariners with the academic and technical training and skills they need to fulfill their duties. Undersea medical officers at NSMRL and other commands on the base assess submariners and divers, who must meet strict medical standards to serve and to participate in high-risk training such as pressurized submarine escape. The submariner duty assessment uses a screening test developed, administered and scored by NSMRL to determine psychological suitability for submarine duty. The base is also home to a 37-foot-tall, 84,000-gallon submarine escape training tower.
What are the special considerations when dealing with submarines and submariners?
Any crew member in a submarine can involuntarily become a diver if the submarine becomes disabled or a fire breaks out and the boat sinks or becomes pressurized. Most submariners don’t go through diver training, but many of them experience pressurized submarine escape training that involves a 15-foot free ascent as well as a 37-foot buoyant ascent in a special survival suit. A research program at NSMRL focuses on ways to improve the survivability of submariners in a disabled submarine.
Other special considerations for submariners include nutritional and physical fitness challenges, atmosphere contaminant exposures in the enclosed environment of a submarine, disruption of the circadian cycle due to the loss of day-night cues, and the social and psychological aspects of being in a confined space during long operations.
I have worked extensively on the physiological and medical challenges of submarine escape, survival and rescue. One of my current projects focuses on establishing new biomarkers for pulmonary oxygen toxicity (POT), which may be of concern to submariners exposed to prolonged periods of hyperbaric air in a disabled submarine or in divers conducting prolonged decompression treatment using 100 percent oxygen.

You presented parts of your work on POT at international conferences this year. What are the unsolved questions regarding lung oxygen toxicity, and why are they relevant?
POT can be a mission-limiting factor for military combat diving operations. If we can increase the amount of oxygen and reduce the amount of inert gas in our breathing mixtures, we can reduce the amount of decompression stress on the diver and thus potentially reduce the decompression obligation for a given dive profile. Unfortunately, breathing a high partial pressure of oxygen while too deep or for too long can result in central nervous system oxygen toxicity or in POT, respectively. Susceptibility to POT is highly variable between subjects, and there are currently no good biomarkers to predict or assess how individuals will react to the oxidative stress on the lungs before the onset of POT symptoms.
We currently measure the effects of POT via pulmonary function tests such as spirometry, but spirometry is not a very sensitive test for POT. Subjects can often produce normal spirometry values despite experiencing severe symptoms of POT. In our most recent study, we looked at impulse oscillometry, which measures the reactance and resistance of the respiratory system. This measure of lung function proved to be a much more sensitive measure than spirometry for detecting the early onset of POT.
To find a noninvasive biomarker to assess oxidative stress in the lungs, we have studied changes in expired nitric oxide (NO) in response to a prolonged oxygen dive. In earlier work we found that expired NO decreases in accordance with the duration of the dive as well as the concentration of oxygen breathed. We recently tested the accuracy of an empirically derived model to predict changes in exhaled NO based on the oxygen dose of the dive profile. Our results showed excellent agreement between the predicted and actual mean NO changes following high hyperoxic dives. Furthermore, we found that individuals with low expired NO levels before a given dive appear to have an increased likelihood of experiencing oxygen toxicity symptoms during repeated provocative hyperoxic exposures.
Does your research apply to recreational or technical divers?
One area of research that is of interest to both recreational and technical divers is the influence of carbon dioxide (CO2) on cognitive function. I was a subject in a 1986 study looking at underwater exercise and changes in breathing mechanics during hyperbaric chamber dives on air to 165 feet of seawater (fsw). The narcotic sensation while exercising hard at depth changed based on the level of CO2 buildup (retention) during the experiment. It progressed from an enjoyable experience to feelings of apprehension, which quickly transitioned to a carefree attitude and significantly impaired judgment. Several other subjects who conducted the same experiment also exhibited similar symptoms but stopped the exercise early due to feelings of panic. Some subjects reported tunnel vision toward the end of the exercise.

This early personal experience prompted me to research the effects of CO2 on cognitive function while at Simon Fraser University. In later research at the Naval Medical Research Institute, we found that the CO2 sensing capability of most divers is bad, and most of us have little awareness of the physiological and cognitive effects of CO2 until levels reach high concentrations.
The breathing responses and symptomology during underwater exercise varied significantly when the divers experienced changes in inert gas narcosis, CO2 levels and inspiratory breathing resistance. We found that nitrogen narcosis tended to reduce the perception of respiratory effort during exercise and that individual divers showed a wide range of breathing responses to respiratory loading and inspiratory levels of CO2. Through these experiments with heavy work at depth, we witnessed CO2 defenders who increased their breathing to try to prevent their levels of CO2 rising during underwater exercise and who showed obvious signs of breathing distress.
On the opposite end of that spectrum were the CO2 retainers, who had a blunted breathing response to underwater exercise in which they would let CO2 build up within their bodies and were less aware of their physiological situation. High levels of CO2 could lead to a sudden loss of consciousness. Understanding the effects of CO2 narcosis is important for both recreational and technical divers who may retain CO2 due to conducting heavy work at depth or situations in which a CO2 scrubber fails in a closed-circuit rebreather. Some individuals may have no warning before they pass out. We do not completely understand whether these differences in breathing responses and CO2 perception are hardwired or can change with training.
What is your next research focus?
I am investigating new ways to monitor contaminants in the submarine atmosphere. We need to think about the materials used in a submarine and what equipment is on board. Some materials might offgas and possibly release toxic substances or contaminants over long periods during a submarine patrol. In an environment where the worker goes home after eight hours, there is a respite from contaminant exposure, unlike for a submariner who has to live and work within the same recirculating atmosphere around the clock during a patrol with only sporadic surfacing for renewal of the atmosphere. While NSMRL’s ongoing Submarine Atmosphere Health Assessment Program has shown that we expect the submarine atmosphere to be safe, the new individual passive dosimeters we are investigating will allow us to more accurately monitor long-term exposure to various air contaminants to ensure the atmosphere remains within existing guidelines.

Another area of active research by several investigators at NSMRL involves combining techniques for using artificial intelligence for data analytics with new technologies, personal wearable devices and noninvasive monitoring of physiological status to predict when fatigue or stress levels affect performance (such as vigilance and situational awareness) on submarine-related tasks.
The effects of the gut microbiome on health and wellness have recently received international interest. New research suggests that the gut microbiome has a significant influence on the brain, and there seems to be two-way communication between the brain and the gut microbiome. Many factors such as diet and sleep schedules can affect the gut microbiome, especially in a submarine where fresh food is limited and sunlight, which provides day-night cues for circadian alignment and vitamin D, is scarce. NSMRL researchers are embarking on a study to look at the impact of a prolonged submarine deployment on a submariner’s gut microbiome. Findings from this study may point to novel ways in which we can enhance a submariner’s health and well-being during a patrol by providing targeted nutritional supplements or probiotics to improve their microbiome.
Do you still dive?
I was certified by the National Association of Underwater Instructors (NAUI) in 1987 while I was working on my master’s thesis in Canada. In 2001 I trained as a U.S. Navy diver at the U.S. Naval Diving and Salvage Training Center in Panama City, Florida. The knowledge I gained and the ability to conduct dives at the commands where I have worked were invaluable, especially when troubleshooting my experiments and understanding the various stressors that military divers may encounter. We have an active Navy dive crew assisting with dive research protocols and diving regularly to maintain certifications, but I must admit that although I still enjoy diving, dives just for fun have become rare.
© Alert Diver — Q1 2020