What should I consider when I return to diving after a joint replacement?
Joint replacement is becoming more common, increasing our quality of life and scope of activity as we age. There are several aspects to consider when returning to diving after a joint replacement, including the risk of damage to the replaced joint, emergency response and the risk of decompression sickness (DCS). Remaining physically active is vital for our general health and important for maintaining bone quality. Better bone quality may help improve stability of a replaced joint, but too much of the wrong activity can cause wear and tear, fracture, loosening and destabilization of the implant and may require surgical revision. Survey studies and consensus recommendations of orthopedic surgeons show that most surgeons recommend low- to moderate-intensity physical activities — such as walking, swimming or cycling — after joint replacement. They discourage high-impact or contact activities such as running, soccer, football and hockey.
Any return to physical activity after surgery depends on complete recovery. Your surgical incisions need to be completely healed, and any complications such as infections must be resolved. To safely dive, you must be able to lift and carry your equipment without any limitations due to pain or restriction in motion. Pain medications that may impair your ability to respond to changes underwater could cause injury or even death to you or your fellow divers in an emergency. Even after you have recovered from the surgical procedure, you’ll need to have also recovered your strength and endurance to deal with any emergency situation that may arise.
A theoretical increase in DCS risk may also warrant postponing diving. Any condition in which blood flow to tissue or joints is compromised could hypothetically impair inert gas elimination and perhaps increase the risk of DCS at surgical sites. At this time, however, there are no objective data to support or quantify an increased risk of DCS at well-healed surgical sites without complications. Returning to diving after joint replacement isn’t necessarily straightforward and should always be assessed on a case-by-case basis. Once your surgeon and a physician with an understanding of dive medicine clear you for diving, we recommend a gradual return. Start in a controlled environment by swimming in a pool with fins, then work your way up to diving in a pool, then eventually move to open water. As with diving after an injury, there is no guarantee that you won’t reinjure the joint or be at increased risk to develop DCS, so diving conservatively is a good idea.
— Kaighley Brett, M.D.
I’m getting a new tattoo on my thigh. Is it safe for me to go diving two days later?
Your tattoo artist will tell you how to properly care for the site of the tattoo and how to prevent infection. The general recommendation is to avoid immersing your tattoo in water — other than showering — until the area has healed (the skin is no longer flaking), which can take several weeks. Going diving two days after getting a tattoo is not recommended due to the risk of infection. As with any wound, be sure healing is complete before you dive.
— Marty McCafferty, EMT-P, DMT
I am starting an antianxiety medication, sertraline, and am wondering if it is safe for me to dive while on this medication?
There are few research studies on the effect of medications in the dive environment, but current information suggests that most medications act the same way underwater as they do on land. They are metabolized the same and, as far as we know, are not affected by elevated partial pressures.

The more significant concern about diving is not the medication itself but rather the underlying condition the medication is treating. I’m sure you can appreciate that a history of anxiety might potentially compromise one’s safety underwater. Your treating physician is your best resource for determining if diving will be a safe activity for you. Provided the condition is well-controlled, you know and avoid anxiety triggers and you have been on the medication for more than 30 days, diving should not present a problem. Again, your doctor needs to make this decision since he or she is accepting the liability by signing your clearance form.
One thing to note is that if you continue your diving education and pursue advanced certifications, your depth limits will increase. Deeper depths involve an increased risk of nitrogen narcosis. Most divers describe narcosis as a carefree, euphoric feeling. This can compromise dive safety because divers may be less able to monitor their depth, dive time, gas consumption, etc. Since some mood-stabilizing medications may have similar effects, there is a theoretical risk of a synergistic effect between nitrogen narcosis and mood stabilizers. This effect has not been formally studied but is a common concern among physicians trained in dive medicine.
Please share this information with your doctor, and let us know if you have additional questions or concerns.
— Lana Sorrell, EMT, DMT
I recently dived at Sipadan Island, where divers are not allowed to wear gloves. At one point I accidentally brushed my hand against something that stung me. I didn’t see any fire coral or wildlife in proximity, and I didn’t experience any immediate redness or rash. One week after returning home, however, I developed a raised red rash with clustered, firm, small, round, red bumps where I had been stung. Sometimes the rash itches, and at other times it is tender to the touch, similar to a burn. It has worsened since I first noticed it two days ago; topical cortisone and tea tree oil have soothed but not diminished it. What could have caused my rash, and how should I treat it?
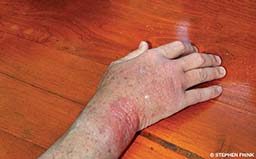
It is impossible to determine precisely what stung you, but your symptoms are consistent with an injury from a sponge, jellyfish or hydroid. Hydroids may attach to any solid structure in the ocean and can be found on mooring lines and other objects.
Initial treatment of these types of stings consists of washing the area of contact with salt water, applying vinegar and treating pain with hot water (as tolerated). It is common for the rash to improve and then get worse again before it heals. At this point in your injury, apply topical steroids, and use heat to treat pain. If you see no improvement in a week or two, see a doctor; you might need oral steroids. The doctor will not need to know what organism stung you and can treat the wound like any other contact dermatitis.
— Travis Ward, EMT-P
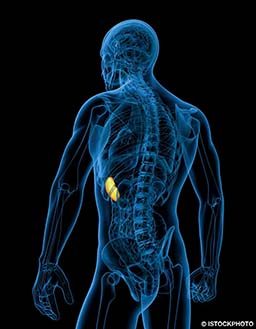
I’ve read online that having a spleen is important for diving. I had mine removed five years ago after a traffic accident. If I dive, am I at increased risk of injury?
The spleen, which stores extra red blood cells (erythrocytes), is not necessary for diving and certainly not for scuba diving. Research shows that when marine mammals hold their breath and make a dive, the resulting complex physiological reaction to apnea will compress the spleen, releasing more erythrocytes into circulation. This process is believed to at least temporarily increase the number of available oxygenated red blood cells and possibly increase the duration of the dive. It is suggested that this same phenomenon occurs in human breath-hold divers (freedivers). Scuba divers breathe compressed air that they take with them to depth — they do not hold their breath. The absence of a spleen is not known to increase injury risk for scuba divers or breath-hold divers.
— Marty McCafferty, EMT-P, DMT
| © Alert Diver — Q4 2018 |