Lesser-known forms of decompression sickness (DCS) can be easily misinterpreted or discounted by affected divers, regardless of their experience level. Kelly, who has a Master Scuba Diver Trainer rating from the Professional Association of Diving Instructors (PADI), experienced some unusual pain and swelling after her first technical dives, but DCS wasn’t the first condition she suspected. Despite the confusing presentation of her DCS symptoms, DAN® was there for this seasoned dive professional.
For months Kelly had been preparing for her technical sidemount diving certification; she was ready to tackle the classroom, handle multiple gas cylinders and complete 12 dives in six days. Now in her early 50s, Kelly has more than 500 dives under her weight belt and is in very good physical condition.
The technical diving course started in shallow water but quickly progressed with deeper and longer dives. Kelly had experienced skin DCS following repetitive deep dives along Florida’s Gulf Coast the previous year, so she was especially cautious going into these dives: She made a point of hitting her decompression stops exactly as her late-model multigas dive computer prescribed.
The course progressed from two shallow dives to 29 feet on air, to three nitrox dives to 90 feet, to two dives that introduced 100 percent oxygen as the decompression gas mix — first to 95 feet for 42 minutes and then to 119 feet for 67 minutes.
After her seventh dive of the course, Kelly’s upper left arm became markedly sore; she said it felt like someone had punched her in the bicep. The skin was uncharacteristically taut, feeling uneven and warm to the touch. She was placed on 100 percent oxygen for 20 minutes but displayed no additional symptoms typical of DCS. Her arm pain and swelling were chalked up to trauma, possibly incurred during a collision on her trip up the boat ladder in rough seas, or a bite or sting, so she kept diving.
She continued training, but the pain and swelling to her left upper arm worsened and spread to her left breast. The consensus aboard the dive boat was that Kelly had suffered a hematoma to the left bicep during her dive ladder encounter, but the absence of discoloration (bruising) to the area seemed to contradict this assessment.
Now four days and five deep, long training dives after her symptoms’ onset, Kelly’s symptoms were worsening; her fingers were tingling, and her chest felt tight. After confusion and visual disturbances set in, she received oxygen for 30 minutes on the boat ride back to shore and was immediately transported to a local urgent care facility. Upon preliminary examination, the attending physician directed her to the nearest hyperbaric chamber at Mariners Hospital in Tavernier, Florida, in the upper Keys.
While en route to the hospital, Kelly’s husband called the DAN Emergency Hotline; after hearing a quick explanation of her symptoms, Marty McCafferty, EMT-P, DMT, suspected Kelly was suffering from lymphatic DCS. He thought a nitrogen bubble might be blocking Kelly’s lymphatic system, creating a backup of lymph fluid into her upper arms and chest.
The mention of suspected DCS at the Mariners Hospital reception desk set things into immediate motion, and Kelly was whisked into an emergency treatment bay. Within minutes, high-flow intravenous fluids and oxygen were administered, a blood panel was drawn, a chest X-ray was taken, and the on-duty hyperbaric technician arrived for a preliminary evaluation, with the hyperbaric physician following suit.
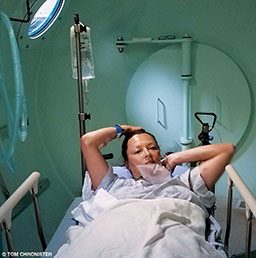
Once a diagnosis was made and lung barotrauma was ruled out, Kelly was wheeled to the hyperbaric chamber, where she underwent the five-hour U.S. Navy Treatment Table 6, a standard of care for DCS. She was discharged after hyperbaric treatment, and over the next several days her swelling dissipated and her neurological symptoms never returned. Once cleared, she flew home to California and followed up with a hyperbaric physician there who cleared her to dive after a four-week hiatus.
In Hindsight
Kelly’s upper-extremity swelling was consistent with lymphatic DCS but a type not highlighted in some dive training manuals. Unfortunately, the most common symptoms represent only a partial list of potential DCS complications; lymphatic concerns such as regional swelling can occur, but it ranks 13th out of the 15 most common initial manifestations of DCS.
This obscure gap in knowledge prevented a group of seasoned dive professionals (including Kelly and her husband) from attributing her symptoms to DCS, not for just a few minutes, but over several days. While this unusual presentation of symptoms excluded the key indicators of DCS, her symptoms did not fool the DAN medical information specialist. A phone call to DAN should have been the first step in managing this case of DCS.
Kelly’s dives were deep and long, but they did not violate any dive plans or protocols: She is just that rare diver who cannot rely on widely accepted decompression algorithms to avoid DCS. To mitigate future risks, she will change her decompression algorithm to a more conservative setting and plans to dive with nitrox.
Medical bills for a trip to the emergency room and a hyperbaric chamber ride are significant, but between Kelly’s personal medical insurance and her DAN Guardian dive accident insurance plan, her expenses were covered. Mariners Hospital directly billed both insurance companies, leaving Kelly with no medical payment follow-up.
From helping pinpoint a diagnosis, to frequent follow-ups, to final medical payments, DAN was there for Kelly.
© Alert Diver — Q1 2019