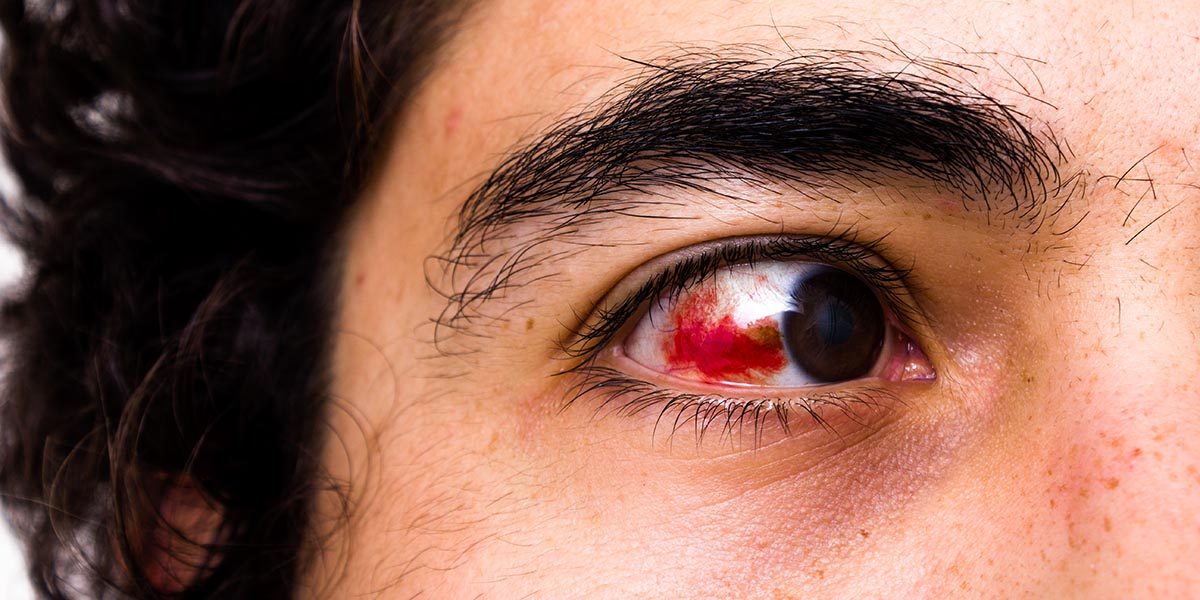
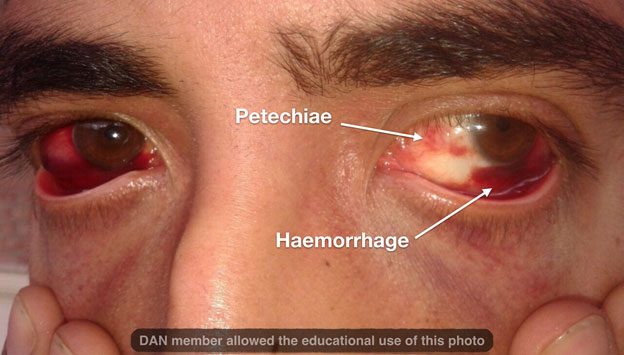
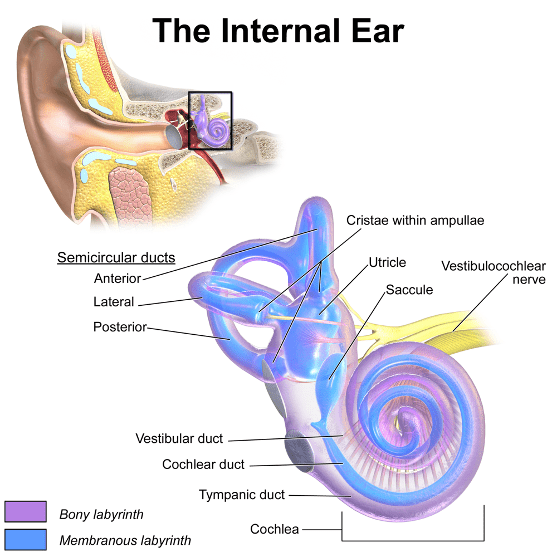
Decompression illness, or DCI, is associated with a reduction in the ambient pressure surrounding the body. DCI encompasses two diseases, decompression sickness (DCS) and arterial gas embolism (AGE). DCS results from bubbles in body tissues causing local damage. AGE occurs when bubbles enter arterial circulation, traveling through the arteries and potentially causing tissue damage by blocking blood flow at the small vessel level.
Who Gets Decompression Illness?
Decompression illness affects scuba divers, aviators, astronauts and compressed-air workers. The main risk factor for DCI is a reduction in ambient pressure, but other risk factors will increase the likelihood of DCI occurring. The known risk factors for divers are deep or long dives, cold water, heavy exercise at depth, and rapid ascents.
Rapid ascents contribute significantly to the risk of AGE. Other factors that may increase DCI risk but lack conclusive evidence of association are obesity, dehydration, heavy exercise immediately after surfacing, and pulmonary disease. We don’t yet fully understand possible individual risk factors. Some divers get DCI more frequently than others despite following the same dive profile.
Almost any dive profile can result in DCI, no matter how safe it seems. The risk factors, both known and unknown, can influence the probability of DCI in many ways. Evaluation of a diver for possible decompression illness is done on a case-by-case basis. The diver’s signs, symptoms and dive profiles are all considered when making a diagnosis.
Decompression Sickness
DCS (also called the bends or caisson disease) results from inadequate decompression following exposure to increased pressure. In some cases, it is mild and not an immediate threat. In other cases, a serious injury occurs. The sooner the treatment of an injury begins, the better the chance for a full recovery.
During a dive, the body tissues absorb nitrogen (and/or other inert gases) from the breathing gas in proportion to the surrounding pressure. As long as the diver remains at pressure, the gas presents no problem. If the pressure is reduced too quickly, the nitrogen may come out of solution and form bubbles in the tissues and bloodstream. Bubbles may occur as a result of violating prescribed limits, but it can also happen even when following accepted guidelines.
Bubbles forming in or near joints are the presumed cause of joint pain (the bends). With high levels of bubbles, complex reactions can take place in the body. The spinal cord and brain are usually affected, causing numbness, paralysis, impaired coordination and disorders of higher cerebral function. If large numbers of bubbles enter the venous bloodstream, congestive symptoms in the lung, and eventually circulatory shock, can occur.
Arterial Gas Embolism
If a diver ascends without exhaling, air trapped in the lungs expands and may rupture lung tissue. This injury, called pulmonary barotrauma, involves release of gas bubbles into the arterial circulation. Circulation distributes them to body tissues in proportion to the blood flow. Since the brain receives the highest proportion of blood flow, it is the main organ in which bubbles may interrupt circulation if they become lodged in small arteries.
This circulation interruption is AGE, considered the more serious form of DCI. The diver may have made a panicked ascent or held their breath during ascent. However, AGE can occur even if the ascent was completely normal. Pulmonary diseases such as obstructive lung disease may increase the risk of AGE.
A diver may surface unconscious and remain so or lose consciousness within 10 minutes of surfacing. These cases are true medical emergencies and require rapid evacuation to a treatment facility.
AGE may involve minor symptoms of neurological dysfunction, such as sensations of tingling or numbness, weakness without obvious paralysis, or complaints of difficulty in thinking but no apparent confusion. In these cases, there is time for a more thorough evaluation by a diving medical specialist to rule out other causes.
Like DCS, mild symptoms may appear to be due to causes other than diving, which can delay treatment. Symptoms may resolve spontaneously, and the diver may not seek treatment. The consequences of this are similar to untreated DCS. Residual brain damage may occur, making it more likely there will be residual symptoms after a future AGE — even after treating the later instance.
Manifestations
DCS
The most common manifestations of DCS are joint pain and numbness or tingling. The next most common are muscular weakness and inability to empty a full bladder. Severe DCS is easy to identify because the signs and symptoms are apparent. However, most DCS manifests subtly with a minor joint ache or paresthesia (an abnormal burning or tingling sensation) in an extremity.
Signs and Symptoms
DCS
- Unusual fatigue
- Skin itch
- Pain in joints or arm, leg or torso muscles
- Dizziness or vertigo
- Ringing in the ears
- Numbness, tingling and/or paralysis
- Shortness of breath
- A blotchy rash
- Muscle weakness or paralysis
- Difficulty urinating
- Confusion, personality changes or bizarre behavior
- Amnesia
- Tremors
- Staggering
- Coughing up bloody, frothy sputum
- Unconsciousness or collapse
Note: Signs and symptoms usually appear within 15 minutes or up to 12 hours after surfacing. In severe cases, symptoms may appear before surfacing or immediately afterward. Delayed onset of symptoms is rare but can happen, especially if air travel follows diving. In many cases, these symptoms are ascribed to another cause such as overexertion, heavy lifting or even a tight wetsuit. Sometimes these symptoms remain mild and resolve by themselves, but they may increase in severity until it is obvious that something is wrong and help is needed.
AGE
- Dizziness
- Visual blurring
- Areas of decreased sensation
- Chest pain
- Disorientation
- Bloody froth from mouth or nose
- Paralysis or weakness
- Convulsions
- Unconsciousness
- Cessation of breathing
- Death
Preventing Decompression Illness
DCS
Recreational divers should dive conservatively, whether they are using dive tables or computers. Experienced divers sometimes select a table depth (rather than actual depth) of 10 feet (3 meters) deeper than called for by standard procedure. This practice is recommended for all divers, especially when diving in cold water or under strenuous conditions. Divers should be cautious about approaching no-decompression limits, especially when diving deeper than 100 feet (30 meters).
Avoiding the risk factors described above will decrease the risk of DCS. Flying or other exposure to altitude too soon after diving can also increase the risk of decompression sickness as explained in Flying After Diving.
AGE
Always relax and breathe normally during ascent. Lung conditions such as asthma, infections, cysts, tumors, scar tissue from surgery, or obstructive lung disease may predispose a diver to AGE. If you have any of these conditions, consult a physician with experience in diving medicine before you dive.
Treatment
The treatment for decompression illness is recompression. Early management of AGE and DCS is the same. It is essential that a diver with AGE or severe DCS to be stabilized at the nearest medical facility before being transported to a chamber.
Early oxygen first aid is essential and may reduce symptoms, but this should not change the treatment plan. Symptoms of AGE and severe DCS often resolve after breathing oxygen from a cylinder, but they may reappear later. Always contact DAN or a physician trained in dive medicine in cases of suspected decompression illness — even if the signs and symptoms appear resolved.
Delays in seeking treatment elevate the risk of residual symptoms. Over time the initially reversible damage may become permanent. After a delay of 24 hours or more, treatment may be less effective, and symptoms may not respond. Even if there has been a delay, consult a diving medical specialist before making any conclusions about possible treatment effectiveness.
After Treatment
There may be residual symptoms after treatment. Soreness in and around an affected joint is common and usually resolves in a few hours. If the DCI was severe, there could be significant residual neurological dysfunction. Follow-up treatments, along with physical therapy, can help. The usual outcome is eventual complete relief from all symptoms with prompt treatment.
With severe DCS, you may have a permanent residual effect such as bladder dysfunction, sexual dysfunction or muscular weakness, to name a few.
In some cases of neurological DCS, there may be permanent damage to the spinal cord, which may or may not cause symptoms. However, this type of injury may decrease the likelihood of recovery from a subsequent bout of DCS.
Untreated joint pain that subsides could cause small areas of bone damage (osteonecrosis). If this happens through repeated instances of DCS, there may be enough damage to cause the bone to become brittle, or for joints to collapse or become arthritic.
Responding to DCI
Determine the Urgency of the Injury
Make an initial evaluation at the dive site. You can suspect decompression illness if you notice any of the signs or symptoms listed above within 24 hours of surfacing from a dive. While waiting for professional medical care or evacuation, take as detailed a history as possible and try to evaluate and record the diver’s neurological status. Base your response on one of these three categories depending upon the symptoms: emergency, urgent or timely.
If necessary, you can administer first aid within the scope of your training, as described below.
Emergency
Symptoms are severe and appear within an hour or so of surfacing. The diver may lose consciousness. Symptoms might progress, and the diver is obviously ill. The diver may be profoundly dizzy or have trouble breathing. Neurological symptoms may manifest as altered consciousness, abnormal gait or weakness.
If necessary (e.g., if the diver isn’t breathing and has no pulse), begin CPR and take immediate action to have the diver evacuated. Check for foreign bodies in the airway. If they need ventilatory or cardiac resuscitation, the injured diver should be lying on their back. Vomiting in this position is dangerous; if it happens, turn the diver to the side until the airway is clear and resuscitation can resume in the supine position. While awaiting evacuation, take as detailed a history as possible and try to evaluate and record the diver’s neurological status.
Use supplemental oxygen while administering breaths to increase the percentage of oxygen breathed by the injured diver. Even if CPR is successful and the diver regains consciousness, continue administering 100 percent oxygen until the diver arrives at a medical facility and health care professionals assume care.
Urgent
The only noticeable symptom is severe pain that is unchanging or has progressed slowly over a few hours. The diver does not appear to be in distress except for the pain, and the neurological signs and symptoms are not evident without a careful history and examination.
Administer 100 percent oxygen and give fluids by mouth. Do not attempt to treat the pain with analgesics until advised to do so by medical personnel. Continue providing oxygen until arrival at the medical treatment facility.
Timely
Symptoms are either not visible or have progressed slowly for several days. The main signs or symptoms are vague complaints of pain or an abnormal sensation, which could indicate something other than DCI. Obtain as complete a diving history as possible and do a neurological evaluation. Then go to the nearest medical facility for evaluation.
Get the Dive History
If possible, obtain and document the following information for all suspected cases of decompression illness:
- All dives (depth, time, ascent rates, surface intervals, breathing gases) for 48 hours preceding the injury. Also note problems or symptoms at any time before, during or after the dive.
- Symptom onset times and progression after surfacing from the last dive
- All first aid measures (including times and method of emergency oxygen delivery) and their effect on symptoms
- Results of an on-site neurological examination
- All joint or other musculoskeletal pain including location, intensity and changes with movement or weight-bearing maneuvers
- Description and distribution of any rashes
- Any traumatic injuries before, during or after the dive.
On-Site Neurological Examination
Information regarding the injured diver’s neurological status will be useful to medical personnel. Examination of an injured diver’s central nervous system soon after an accident may be valuable to the treating physician.
The exam is easy to learn, and individuals with no medical experience can perform it. Do as much of the examination as possible, but do not let it interfere with prompt evacuation to a medical treatment facility. (Find the instructions at On-Site Neurological Examination.)
Medical Evaluation
Call local EMS to get the diver to the nearest medical facility.
Returning to Diving after DCI
For recreational divers, whose livelihood is something other diving, a conservative approach will help minimize the chance that a diving injury will recur.
- After pain-only DCI without neurological symptoms, you can consider a return to diving after a minimum of two weeks.
- With minor neurological symptoms, consider returning after six weeks.
- If you had severe neurological symptoms or have any residual symptoms, you should not return to diving.
You should always consult with a physician before returning to diving. Even if symptoms were not severe and they resolved completely, if you have had multiple instances of decompression illness, you must make special considerations. If you are getting DCI when other divers who dive the same profile are not, you may have elevated susceptibility. In these cases, consult a dive medicine specialist to determine if you can safely resume diving.
Ed Thalmann, M.D.